
A young baby girl, six months of age, was brought into a doctor’s office two years ago. The child, daughter of Kristie Tait, presented with hives and rashes that seemed to come and go. The child cried from pain and frantically grabbed at her face, legs, or anywhere else on her body in an attempt to take off what was hurting her. The primary care provider did not necessarily believe this called for urgency; instead, the baby girl was eventually and indefinitely denied medical care in her region due to the stigma and controversy surrounding what she would later be diagnosed with.
The child’s pediatrician initially declared the girl was experiencing allergies or eczema until more symptoms presented (tests ruling out allergies), and was sent to the University of Alberta Hospital in Edmonton Canada, where the family was told the child fit the criteria of Morgellon’s disease–a condition Mrs. Tait was at the time unfamiliar with. The child’s siblings and father also presented with similar symptoms of “coffee grounds” expelling upon exfoliation. The doctor with the University of Alberta Pediatric Infectious Disease, and the Edmonton Clinic Health Academy, confirmed black specks were coming out of the lesions.
Although the doctor initially offered regular consultation and advice, he refused to offer her any treatment and eventually ceased responding to the mother’s emails after she voiced her concern over her daughter undergoing repeated scabies treatments. The child and family were treated a reported 12 times for the parasite (an easy-to-treat condition with topical lotion) and to no avail. Mrs. Tait was also denied treatment by a nurse practitioner at a hospital in Cold Lake, and was refused an appointment by a clinic in Bonnyville, to which she was referred, for reasons not made clear.
Since the Centers for Disease Control and Prevention (CDC) investigation and study in 2008 of Morgellon’s disease, which came to an abrupt and unexpected end, people around the world voiced their disbelief and upset with an unsupported conclusion of delusional parasitosis (DP). This is now more commonly called unexplained dermopathy due to the lack of scientific support of DP criteria in Morgellon’s patients.
The authors of this study are listed as Michele L. Pearson, Joseph V. Selby, Kenneth A. Katz, Christopher R. Braden,Virginia Cantrell, Monica E. Parise, Allen W. Hightower, Mark L. Eberhard, Arthur Papier, Christopher D. Paddock, Michael R. Lewin-Smith, Victor F. Kalasinsky, Felicia C. Goldstein, Brian Lewis, Sarita Motipara—a uniquely large research team for a relatively minute sample scale.
Dr. Wymore and staff with the Oklahoma State University (OSU) published a letter (attached) for every sufferer to take to their physician. He outlined the differences between Morgellon’s patients and sufferers of delusional parasitosis.
Furthermore, the greatest impact the CDC study had on the world effects those most vulnerable: children and the chronically ill.
Support for the Stigma
Because of the bizarre and unprecedented characteristics of the symptoms related to Morgellon’s disease, patients desperately attempt to collect samples for their doctors to analyze under the microscope. Most doctors, however, choose not to analyze these samples, but have commonly been found to tell the patients that the “specimens” are textile in nature. These “textile” fibers, unfortunately, have been found in deep-tissue biopsy, reported by researchers at OSU, and therefore do not support the claim that the filaments attached to wounds strictly come from clothes or by inadequately cared-for abrasions.
OSU staff advise physicians not to presume their patients are mentally-ill because of their behavior or inclination to bring samples in for professional examination. These patients have been told by one of the “de facto national authorities” that their condition is “all in their heads.” However,as found in the general public ,there actually are patients with delusions of parasitic infestation, and they are suffering greatly.
 It is not just that baby girl, however, who faces a struggle obtaining medical care due to a stigmatized condition. Another patient by the name of, Ed Scherer, is an older gentleman that has been suffering with chronic health issues. He has been turned down repeatedly and even prematurely stigmatized with delusional parasitosis, which likely would not have been in the doctor’s realm of thought without the previously published CDC report. Doctors within the University of Maryland Medical system have forwarded to Mr. Scherer their email correspondence:
It is not just that baby girl, however, who faces a struggle obtaining medical care due to a stigmatized condition. Another patient by the name of, Ed Scherer, is an older gentleman that has been suffering with chronic health issues. He has been turned down repeatedly and even prematurely stigmatized with delusional parasitosis, which likely would not have been in the doctor’s realm of thought without the previously published CDC report. Doctors within the University of Maryland Medical system have forwarded to Mr. Scherer their email correspondence:
“Hi Dr. Edelman,
I think it is delusional parasitosis. Unfortunately, we have seen many such patient in our ID clinic. They always produce “specimens” and photos.
Thank you for NOT scheduling him with us!Thanks, Mariam”
A follow-up was written to Scherer as an apology, but also with a statement saying the doctors at the medical center would not see him as their patient. He was further advised to contact Baltimore Medical Society. No comments from the staff members have been made to the media.
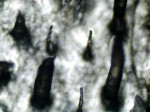 There are many research teams providing overwhelming evidence which supports Morgellon’s disease and the finding of filament producing agents. The National Institutes of Health (NIH) Office of Rare Diseases have stated that they are accepting private questions and comments through Email, and will publish more on Morgellon’s disease as it is comes to be understood. (An independent researcher collected a tissue sample from a patient and photographed at a microscopic magnification of 40x as presented in the above image).
There are many research teams providing overwhelming evidence which supports Morgellon’s disease and the finding of filament producing agents. The National Institutes of Health (NIH) Office of Rare Diseases have stated that they are accepting private questions and comments through Email, and will publish more on Morgellon’s disease as it is comes to be understood. (An independent researcher collected a tissue sample from a patient and photographed at a microscopic magnification of 40x as presented in the above image).
Researchers have revealed much information regarding this syndrome or disease. There is a greater likelihood that multiple agents are affecting humans, but have slipped under the radar for so long due to inadequate diagnostic tools currently utilized.
Though Kathleen Sebelius has left her position as Health and Human Services (HHS) Secretary recently, just this year she led an international meeting in Washington for a private conference and discussion. The topics revolved around failure by many countries in meeting International Health Regulation standards, which was last set many years ago. The meeting also focused much attention on a new Global Health Security Agenda (GHSA).
The GHSA has been established so that laboratories (among other bio-security systems and protocols) can be built and equipped with adequate diagnostics in every country. Financial categories were placed on every nation so that the upper-level gross domestic product (GDP) countries could assist lower-level countries in meeting these new standards. Though the media was not allowed to be present for this conference, some comments were obtained.
Among what was released to the media was a statement regarding the threat of bio-engineered threats–currently undetectable due to the lack of effectiveness in current diagnostics.
A 2011 report in the media from The Telegraph alleged a CDC study was in a peer-review stage, but such a study has not yet been released.
Unfortunately now, it may be harder for people to accept the credibility of researchers at the CDC. Much additional heat has been directed towards CDC staff for alleged Lyme disease mishandling.
There is a major problem, and the stigma will continue to pose a threat to potentially every person around the globe, as they may succumb to the condition that very few medical physicians are willing to accept and treat.
“We still have no help, no treatment, and no compassion from the medical establishment. My daughter is sick. My 10-year-old is sick. Their mom is sick. This is not just a skin issue. It is systemic.”–Kristie Tait. The baby girl who was denied medical care due to this dreaded stigma, takes part in a story that should not ever have to be told in America. It should, indeed, be the last story ever heard of an injustice faced by those in the Western world.
Opinion By Lindsey Alexander
Related: World Health Organization New Public Health Standards , and
Stroke, Meningitis, Alzheimer’s Caused by Lyme Disease [Video]
Sources:
Oklahoma State University
PLOS one
Telegraph
Direct Correspondence: Ed Scherer, Katie Tait, Tobe Mils
Discover more from Guardian Liberty Voice
Subscribe to get the latest posts sent to your email.



4 Responses
I understand that DE for humans will help.
poor girl! i can’t imagine how hard it is to find a doctor who will treat an infant with this. i’ve had morgellons for 3 years. even the LLMDs i’ve contacted want nothing to do with this disease. i’ve resorted to reading pubmed and working out a multi-antibiotic treatment. so far i can say tindamax is crucial, better still, add zithromax and plaquenil. i’m going to rotate in another macrolide to mix it up more. this is the only thing that has completely stopped new filaments, granules and fiber balls from forming. the hard part is dealing with 3 years worth of material under the skin that is now coming out. as anyone with this disease knows, nothing heals until it’s gone.
Morgellons is hard to cure just like Bartonella infections are hard to cure. But it can be done. Read the Bart page first.
I am with the Kentuckiana Lyme Support Group. Morgellon’s disease is very real. It is caused by infection and it takes the right doctor to figure it out. Please contact us on Facebook and we can help you. Thank you for bringing this story to our attention.