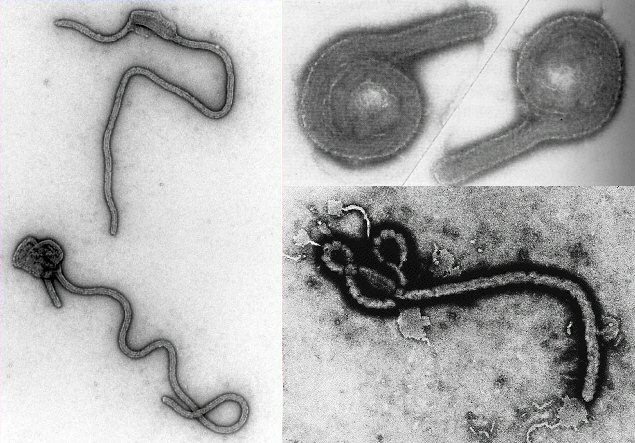
The World Health Organization (WHO) recently released a report which blames the outbreak of the unnamed capricious ebola virus strain on a severe lack of cooperation on the part of the local population, own ignorance regarding the nature of both the deadly Ebola virus and its proper medical treatment combined with a widespread distrust of modern medicine, both its practitioners and its methods, have aided the continued existence of the nearly five month long Ebola outbreak that has killed more than 400 people in West Africa. These findings echo complaints made by many doctors and observers who have worked or are currently working in the area to resolve the crisis. These accounts accuse the locals of actively preventing the work of doctors and other medical personnel out of irrational suspicions, beliefs and customs. The report also cited the relatively free movement across the borders of Guinea, Liberia and Sierra Leone, as well as the numerous border crossings made for commercial purposes including personal travel across borders, as major contributors to the outbreaks which have infected at least 600 people since the first outbreak in Guinea in March.
Since that time the situation has become increasingly worse and the outlook grows grimmer by the day. So grim in fact that WHO called for an emergency meeting in the city of Accra in Ghana. In addition to the health ministers responsible for protecting the public health of the affected countries, 11 other public health ministers from all across the continent, including other West African nations, attended, as did many non-governmental agencies and other stakeholders. These diverse groups discussed and formulated a plan to “get a grip” on the outbreaks which currently show little sign of abating. WHO planned on advocating a “strong response” to the crisis and to encourage continued cooperation between the afflicted nations who, so far, have been unable to stem fully the deadly pathogen’s ever widening reign of terror.
The Ebola virus was first identified in 1976 after two outbreaks in both Sudan and the Democratic Republic of Congo, then known as Zaire. Researchers called it Zaire Ebolavirus in order to distinguish it from similar pathogens, and for good reason. Since that time at least twenty outbreaks have been recorded in Africa, large majority of which involved the the Zaire strain. These incidences occurred mainly in Central Africa’s rural areas, especially places in which humans live in close contact with the many wild animals thought to carry the virus. The reason the current situation in Western Africa has become an issue of international importance is twofold. First, it is likely the ever growing number of both infected and dead, and second, and more importantly, the unique geographical distribution of the outbreaks themselves.
Unlike most of the other outbreaks in the continent’s history, which were confined to small rural areas which were not only at high risk but also lacked access to proper healthcare personnel and facilities, these outbreaks are taking place in both cities and rural areas. Looking over a map of outbreak locations, the disease first spread outward from Guinea and then hopped around and into its southern neighbors Liberia and Sierra Leone, again spreading itself through villages and cities alike. It spread so quickly that by June the situation had become so dire that the director of operations of Medecins Sans Frontieres (MSF), Bart Janssens, declared that the situation was “out of control.” He pleaded with the international community for more support, especially in the form of personnel trained in treating Ebolavirus, noting the ignorance of the locals in treating the disease. In the same article in which they chose to highlight Janssen’s frustration over the ignorance of the local citizens, MSF also pointed out, rather mildly, that locals were certainly “suspicious” of western medical practices, meaning that it was likely distrust of western medicine that kept them from receiving care.
Speaking with Time Magazine, Dr. Van Herp, a physician and MSF member who was in Guinea during that first outbreak in March, described his experiences attempting to treat those infected with the virus. These anecdotes mirror many of the issues identified in the WHO’s report on the outbreaks. For instance, Van Herp recounted being forbidden entry into a village where he was to treat the sick by “aggressive men.” He also mentioned the massive stigma which many in those societies have against those infected with the virus. He claimed that some of the recently diagnosed would actually flee their homes rather than be branded as a carrier of the virus for fear that his neighbors might harm his family members and destroy his property, which Van Herp says is a common practice in certain villages. Meanwhile in other parts of the region, the opposite problem can be found in locals whose distrust or “suspicion” of medical authorities has inspired them to actively oppose attempts at treating Ebola, posing a serious problem for containment. In Sierra Leone the families of Ebolavirus patients decided to liberate their kin from a treatment center, claiming that the former patients needed “traditional medicine” instead of occidental methods.
Like the “aggressive men” who were hording desperately sick people, these individuals were displaying an astounding amount of what can only be called ignorance, as an individual with Ebola is essentially a walking vector for the disease. Western doctors keep Ebolavirus patients in isolation because every single bodily fluid contains the pathogen and can easily infect others who come into contact with them. Incidences like this, where Ebola patients are prevented from seeing doctors by family or friends who distrust the medical established, have motivated at least two of the three countries fighting the outbreaks to take action. Both the governments of Sierra Leone and Liberia have made the “sheltering” or “holding” of Ebola patients a serious crime and have informed their citizens that they will prosecute anyone who trespasses the law.
Another form of ignorance has been noted by observers and those who tend to the sick report tales of increasing belief in superstition and extreme denial of medical science, especially among the inhabitants of rural areas, many of whom refuse to believe that Ebola exists at all, instead blaming witchcraft and other supernatural causes for the disease’s symptoms. Others, falsely believing that there is no chance of surviving the disease will often refuse to seek out treatment, and yet because they are not isolated they can still spread the disease, even after dying their body can still transmit the virus. In fact the high mortality rate among the infected has even fueled rumors that doctors working in the treatment centers, and not the pathogens that they are trying to help the afflicted defeat, are actually executing their patients via lethal injection instead of treating them.
The distrust, the ignorance and of course the sheer severity of Ebola itself has created what the Center for Infectious Disease Research and Policy calls the worst outbreak ever to befall the African Continent. The latest numbers put the death toll at 468. Fortunately now that WHO has formally identified the main contributors to this horrific plague and brought the region’s leaders together with public health organizations from around the globe, they will be able to develop a plan of action that will both educate the ignorant and frightened who have inadvertently spread the disease by fleeing isolation and eschewing western medicine. This should also ease the concerns of those angry and aggressive citizens whose distrust towards trained physicians has doubtless cost many lives, and shall continue to do so unless their governments agree on how to best deter the distrustful, enlighten the ignorant and encourage the fearful.
If they cannot resolve these issues and do away with norms that actively thwart containment efforts, then it seems likely that this deadly virus will expand farther out into other towns, cities, villages and perhaps even other countries. A medical official affiliated with WHO has already gone on record advising other western African nations such as Côte d’Ivoire, Mali, Senegal and Guinea-Bissau to prepare their healthcare systems for possible outbreaks of the disease. Still, the efforts of Liberia, Guinea and Sierra Leone’s healthcare workers along with organizations like MSF, WHO and other international medical societies dedicated to protecting global health should not be dismissed without careful consideration of the power that an allied policy front could bring the struggle against the disease. It is in Accra that the people of western Africa have either been delivered from a future marked by a regional epidemic or doomed to one in which the climate of ignorance, distrust, and fear continues to enable to current the microbial insurgency as its reign of infectious terror, unfettered by a healthcare system which still struggles against the tide of superstitious and unknowing minds clouded by mistrust.
By Andrew Waddell
Sources:
Time
Center for Disease Control World Health Organization
TrustMedecins Sans Frontieres
BBC News All Africa
Center for Infectious Disease Research and Policy
Global Post
International Federation of Red Cross and Red Crescent Societies
Discover more from Guardian Liberty Voice
Subscribe to get the latest posts sent to your email.



One Response
Thanks a lot to WHO team. My organization (Lutheran Development Service in Liberia/Actalliance) is carrying out sensitization and awareness in 10 border communities between Liberia and Guinea sponsored by the Raid Response Fund from Actalliance in Geneva.
The local populace problem is the denier of this deadly Ebola Virus outbreak in African. If WHO can sponsor national organizations/civil society organizations to carry out sensitization and awareness, involing medical workers, school children, religious and traditional leaders in the affected countries then problem will be minimized.
By Vandi V. Kallon