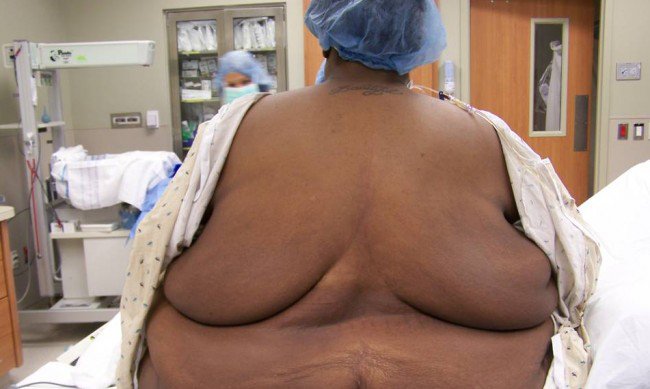
While most care-givers in the medical community are trained to treat their patients with compassion regardless of socioeconomic status, education, sex, religion, or age, one kind of prejudice that may still require addressing is that relating to morbidly obese patients. With obesity and morbid obesity posing an ever-more burgeoning problem in the United States, it is especially important that the medical community overcomes this prejudice so that patients can feel comfortable going to hospitals and other health-care facilities to discuss their health with the people that stand to benefit them the most.
Morbid obesity can be defined in a number of ways. Some consider morbid obesity as having a Body Mass Index score (the quotient of one’s weight in kilograms divided by the square of one’s height in centimeters) of over 40 or more. Others consider 35 to be the cut-off BMI score if a person is also experiencing obesity-related health conditions such as diabetes or high blood pressure. Still others define morbid obesity as weighing 100 pounds heavier that one’s ideal body weight.
People with morbid obesity are likely to face ridicule and discrimination because of their bodies. Many people view morbid obesity as the product of poor personal decisions and/or character flaws. Both judgmental and well-meaning individuals may cause feelings of shame or rejection in a morbidly obese person. In some cases the worst abuses come from loved ones.
Research into the attitudes of members of the medical community found that the healthcare environment is not immune to issues of discrimination and prejudice against patients with morbid obesity. One study published in the journal Obesity Surgery concluded that “the morbidly obese continue to be a forgotten and often mistreated segment of society.”
To begin, many hospitals do not stock equipment capable of servicing morbidly obese patients. Such items include extra large hospital gowns, sturdier chairs and examination tables, and even adequate medical equipment such as over-sized sphygmomanometer cuffs for taking blood pressure.
A survey of 100 third-year medical students revealed that their attitudes towards morbidly obese patients were nearly uniformly negative. Students reported impressions of the morbidly obese as being “unpleasant,” “difficult to manage,” “ugly,” and “having a lack of self-control.” Only in evaluations of honesty were the morbidly obese seen as being equal to people of normal weight or people with moderate obesity. Furthermore, even after completing an educational clerkship that involved working closely with morbidly obese patients, the medical student’s opinions of the morbidly obese did not improve. To the contrary, many of them indicated that the morbidly obese were more “difficult to manage” than they had originally anticipated.
Negative attitudes towards the morbidly obese can result in actions or lack of action that may greatly impact a patient’s health. For instance, when presented with otherwise identical patient histories, psychologists ascribed more mental health pathologies to patients that were obese than to patients of normal weight. The National Association to Advance Fat Acceptance (NAAFA) also reports that doctors spend less time with obese patients, spend less time discussing patient options, and are reluctant to perform health screening procedures such as pelvic exams and cancer screenings.
Can these negative attitudes towards the morbidly obese be amended? A study from 1979 suggests that perhaps one of the best ways for an individual to build empathy and compassion towards the obese is to have one’s own successful experience with weight reduction. In addition there is hope that if issues of obesity were framed as an addiction or compulsive disorder similar to alcoholism, the medical community would be less judgmental of the morbidly obese. Though further research into this matter is necessary, it is vitally important that the medical community learn to embrace patients of all shapes and sizes as needing compassionate care for the promotion of health and wellness.
By Sarah Takushi
Sources
American Journal of Clinical Nutrition
National Association to Advance Fat Acceptance
Obesity Research Review
Discover more from Guardian Liberty Voice
Subscribe to get the latest posts sent to your email.



3 Responses
I couldn’t resist commenting. Exceptionally well written!
The 49ers’ defense was just as bad, allowing Carson Palmer to pick them apart and Chris Johnson to run around and through them.
Back when I was around my peak weight my internist’s PA termed me “morbidly obese” even though my BMI was only about 37. I had a lump in my left breast which turned out to be only a hematoma which resolved itself. But the PA was plainly disgusted by my fatness. Said she: “It’s not surprising that you have such large breasts, since you’re morbidly obese.” Well, now I am thin, but with no intent and no experience of deprivation. Many Doctors are biased against fat patients, and the fatter they are the more they are likely to be ill-served. http://ireport.cnn.com/docs/DOC-968195